Mental health practices across the USA are facing a quiet but significant shift. Patient demand is rising, payer rules are tightening, and documentation requirements are becoming more complex by the day. For therapists, psychiatrists, and behavioral health clinics, managing billing internally often turns into a time-consuming burden that eats into patient care.
That’s where choosing a top outsource mental health billing company becomes more than a convenience—it becomes a strategic move.
This guide breaks down how outsourced billing works in mental health, why it matters, and how to choose the right partner without falling into common traps.
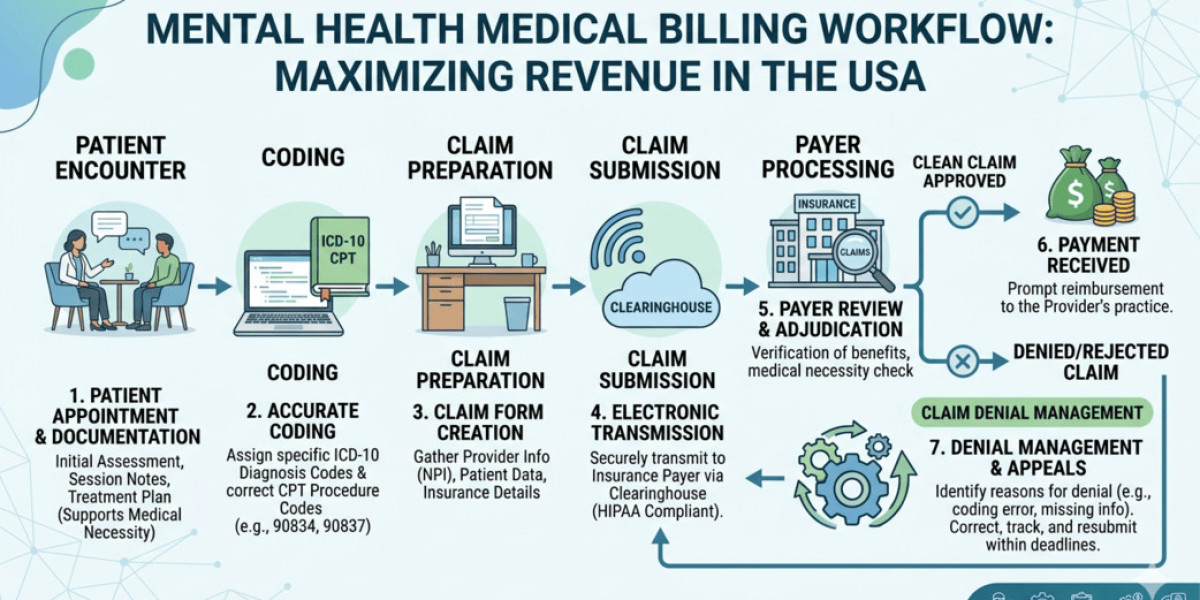
Why Mental Health Billing Is More Complex Than Ever
Mental health billing isn’t just about submitting claims. It involves:
- Frequent policy changes from insurers
- Strict documentation for therapy sessions
- Pre-authorizations for certain treatments
- Coding variations between psychotherapy, psychiatry, and telehealth
Unlike other specialties, behavioral health billing often deals with longer treatment cycles and recurring sessions. This increases the chances of claim denials if even a small error occurs.
That’s why many providers are turning to mental health insurance billing services instead of relying solely on in-house teams.
What Does It Mean to Outsource Mental Health Billing?
When you outsource mental health billing services, you delegate your billing operations to a specialized third-party team. These experts handle everything from claim submission to payment posting.
A reliable mental health billing services agency typically manages:
- Insurance verification
- Coding and claim creation
- Submission and tracking
- Denial management
- Patient billing
- Reporting and analytics
This isn’t just outsourcing work—it’s optimizing your financial workflow.
Key Benefits of Outsourced Mental Health Billing
1. Improved Revenue Flow
A professional mental health billing provider ensures claims are submitted correctly the first time. Fewer errors mean faster reimbursements and fewer denials.
2. Reduced Administrative Burden
Therapists and staff can focus on patient care instead of paperwork. This is especially valuable for small practices.
3. Access to Billing Specialists
A mental health billing specialist understands CPT codes, modifiers, and payer requirements specific to behavioral health.
4. Better Compliance
Regulations in healthcare are strict. A trusted mental health billing and coding company helps maintain compliance with HIPAA and payer guidelines.
Services Offered by the Best Mental Health Billing Agencies
A best mental health billing agency goes beyond basic billing. It becomes part of your operational backbone.
Core Services Include:
- Mental health medical billing services outsourcing
- Claims submission and tracking
- Denial analysis and appeals
- Payment reconciliation
- Financial reporting
Advanced Support:
- Telehealth billing optimization
- Multi-payer handling
- Practice performance insights
Some agencies also combine billing with medical coding services to ensure accuracy at every stage.
Real-World Scenario: Why Outsourcing Works
Consider a mid-sized therapy clinic in Texas. The clinic struggled with:
- 20% claim denial rate
- Delayed reimbursements
- Overworked front-desk staff
After partnering with a mental health billing agency, they:
- Reduced denials to under 8%
- Improved cash flow within 3 months
- Freed up staff to focus on patient intake
This is the kind of transformation a professional mental health billing company can deliver when systems are aligned correctly.
How to Choose the Right Mental Health Billing Company
Not all billing partners are equal. Choosing the wrong one can create more problems than it solves.
Look for These Qualities:
1. Specialty Experience
Choose a provider experienced in mental health medical billing services, not just general billing.
2. Transparency
Clear reporting and communication are essential.
3. Technology Integration
Your billing partner should work seamlessly with your EHR system.
4. Custom Solutions
Every practice is different. Avoid one-size-fits-all solutions.
5. Strong Denial Management
A good mental health billing consultant focuses heavily on reducing denials.
In-House vs Outsourced Billing: A Quick Comparison
| Factor | In-House Billing | Outsourced Billing |
|---|---|---|
| Cost | High (staff, training, software) | Predictable |
| Expertise | Limited | Specialized |
| Scalability | Difficult | Easy |
| Compliance | Risky | Managed |
| Efficiency | Moderate | High |
For growing practices, outsourced mental health billing often delivers better long-term value.
The Role of Coding in Mental Health Billing
Accurate coding is critical in behavioral health. Even minor mistakes can lead to claim rejection.
This is where medical coding services play a vital role. A combined approach using medical billing and coding services ensures:
- Correct CPT and ICD-10 usage
- Proper documentation alignment
- Faster approvals
For example, psychotherapy sessions require precise time-based coding. Errors here can directly impact reimbursement.
Revenue Cycle Management: The Bigger Picture
Billing is only one part of the process. The full financial journey—from patient registration to final payment—is known as revenue cycle management services.
An effective mental health medical billing solution integrates:
- Front-end verification
- Mid-cycle claim management
- Back-end collections
This holistic approach improves financial stability and reduces revenue leakage.
Why Credentialing Matters in Mental Health Billing
Many practices overlook credentialing, but it’s foundational.
Without proper credentialing services, providers may:
- Face claim rejections
- Experience delayed payments
- Lose network opportunities
A billing partner that also supports credentialing ensures providers are properly enrolled with insurers, allowing smoother claim processing.
Signs You Need to Outsource Your Billing
You might benefit from a top outsource mental health billing company if:
- Claim denials are increasing
- Payments are delayed
- Staff is overwhelmed
- Revenue is inconsistent
- Compliance concerns are rising
Ignoring these signs can lead to long-term financial strain.
Future Trends in Mental Health Billing
The industry is evolving quickly. Key trends include:
- Increased telehealth billing complexity
- AI-assisted claim audits
- Value-based care models
- More payer-specific rules
Partnering with a forward-thinking mental health billing companies provider helps you stay ahead of these changes.
Final Thoughts
Outsourcing is no longer just an option—it’s becoming a necessity for mental health practices aiming to scale efficiently in the USA.
Choosing the right billing services for mental health providers can dramatically improve cash flow, reduce stress, and enhance patient care.
Organizations like 247 medical billing services are part of this evolving landscape, offering integrated support that includes:
- medical billing services
- medical coding services
- medical billing and coding services
- revenue cycle management services
- credentialing services
When these elements work together, practices gain more than just financial stability—they gain operational clarity.
FAQs
1. What is the benefit of outsourcing mental health billing?
Outsourcing reduces administrative workload, improves claim accuracy, and speeds up reimbursements by using specialized expertise.
2. How do mental health billing services handle insurance claims?
They verify patient eligibility, code services accurately, submit claims, and follow up with insurers to ensure timely payment.
3. Is outsourced mental health billing secure?
Yes, reputable companies follow strict HIPAA compliance and use secure systems to protect patient data.
4. How much do mental health billing companies charge?
Costs vary, but most charge a percentage of collections or a flat monthly fee depending on services offered.
5. Can small practices benefit from outsourced billing?
Absolutely. Small practices often see the biggest improvements in efficiency and revenue after outsourcing.
6. What should I look for in a mental health billing consultant?
Look for experience in behavioral health, transparent reporting, strong denial management, and technology compatibility.