The landscape of mental healthcare in the USA is evolving rapidly. As demand for therapy, counseling, and psychiatric services rises, so does the complexity of managing administrative tasks—especially billing and credentialing. For many providers, balancing patient care with operational efficiency has become a real challenge.
This is where mental health billing and credentialing services step in—not just as support functions, but as strategic tools that directly impact revenue, compliance, and long-term growth.
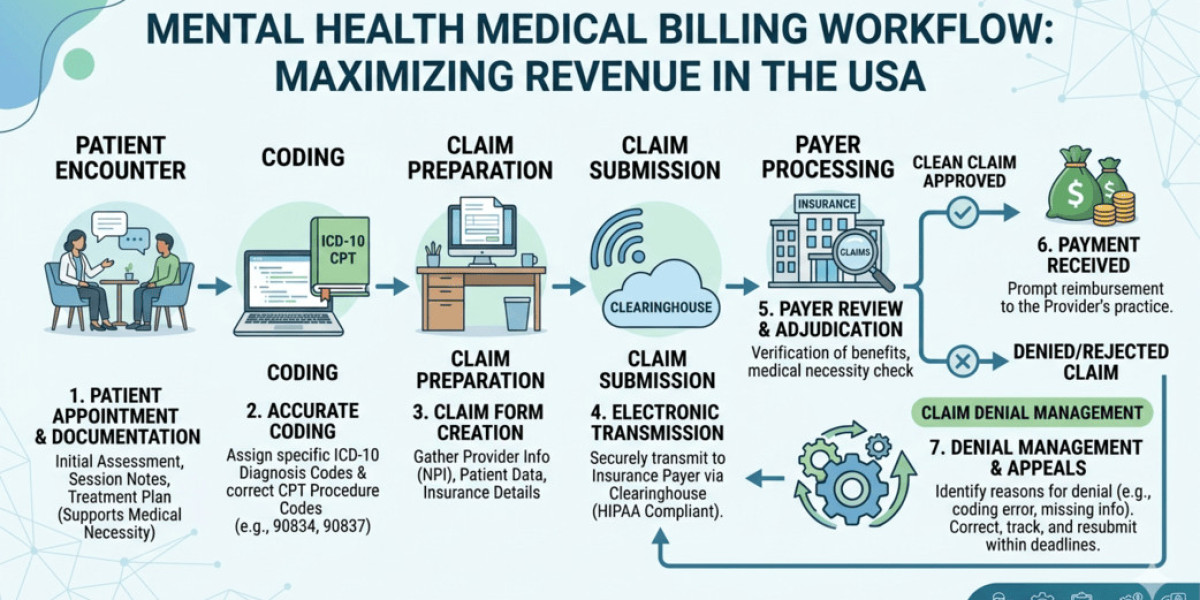
Why Mental Health Billing Is More Complex Than Ever
Billing for mental health providers is not as straightforward as general medical billing. It involves unique coding structures, frequent policy updates, and strict payer requirements.
Some of the key challenges include:
- Frequent changes in insurance policies for behavioral health
- Complex CPT and ICD coding requirements
- Prior authorization hurdles
- Time-consuming credentialing processes
- High claim denial rates
For therapists, psychologists, and clinics, handling billing for mental health services internally often leads to revenue leakage and burnout.
Understanding Mental Health Billing and Credentialing Services
At its core, mental health billing solutions involve managing the entire financial workflow—from patient registration to final payment.
Credentialing services, on the other hand, ensure that providers are authorized to work with insurance companies and receive reimbursements.
Key Components Include:
- Insurance verification
- Claim submission and tracking
- Payment posting
- Denial management
- Compliance monitoring
- Provider credentialing and re-credentialing
When combined, these services create a streamlined system that improves cash flow and reduces administrative burden.
The Role of Medical Billing and Coding in Mental Health
Accurate medical billing for mental health depends heavily on precise coding. Even minor errors can result in denied claims or delayed payments.
Why Coding Matters:
- Ensures compliance with insurance guidelines
- Reduces claim rejections
- Maximizes reimbursement
- Supports audit readiness
Professional medical coding services understand the nuances of psychotherapy sessions, telehealth billing, and medication management codes.
When paired with medical billing services, the entire process becomes more efficient and error-free.
Outsourcing Mental Health Billing: A Smart Move?
Many practices today are turning to outsourced billing for mental health to stay competitive.
Benefits of Outsourcing:
- Access to experienced billing professionals
- Reduced operational costs
- Faster claim processing
- Lower denial rates
- Scalability for growing practices
Instead of hiring and training in-house teams, outsourcing allows providers to focus on patient care while experts handle billing for mental health therapists and clinics.
Real-World Example: A Growing Therapy Practice
Consider a mid-sized therapy clinic in Texas that struggled with delayed reimbursements and frequent claim denials.
After switching to outsourcing mental health billing, they saw:
- 35% reduction in claim denials
- 25% increase in monthly revenue
- Faster insurance approvals
- Improved staff productivity
This highlights how choosing the right mental health billing services can directly impact financial performance.
Medicare and Mental Health Billing
Billing Medicare for mental health services comes with its own set of rules.
Important Considerations:
- Coverage limitations for therapy sessions
- Specific documentation requirements
- Telehealth billing regulations
- Strict coding guidelines
Mistakes in billing Medicare can lead to audits or penalties. This is why many providers rely on specialized behavioral and mental health billing services that understand federal compliance.
Credentialing: The Foundation of Reimbursement
Before submitting claims, providers must be credentialed with insurance networks.
Why Credentialing Services Are Critical:
- Enables providers to accept insurance patients
- Ensures timely reimbursements
- Prevents claim rejections due to network issues
- Keeps provider information updated
Credentialing is not a one-time task—it requires continuous monitoring and renewals. Professional credentialing services help avoid costly disruptions.
Choosing the Best Mental Health Billing Partner
Not all billing companies are the same. Selecting the right partner can make a significant difference.
What to Look For:
- Experience in mental health medical billing
- Transparent pricing (avoid hidden costs)
- Strong reporting and analytics
- Compliance with HIPAA regulations
- Proven track record in denial management
Whether you're searching for a cheap outsource mental health billing company or the best outsource mental health billing and coding services, quality and expertise should always come first.
Technology and Automation in Mental Health Billing
Modern mental health billing solutions are powered by advanced technology.
Features That Matter:
- Automated claim submission
- Real-time eligibility verification
- AI-driven denial prediction
- Integrated EHR systems
- Detailed financial reporting
These tools enhance the efficiency of revenue cycle management services, helping providers stay ahead in a competitive healthcare environment.
How Revenue Cycle Management Drives Profitability
Revenue cycle management is more than just billing—it's a complete financial strategy.
Key Stages:
- Patient registration
- Insurance verification
- Coding and billing for mental health services
- Claim submission
- Payment collection
- Denial resolution
Effective revenue cycle management services ensure that every step is optimized, reducing revenue loss and improving cash flow.
Common Mistakes in Mental Health Billing
Even experienced providers can make costly errors.
Avoid These Pitfalls:
- Incorrect CPT or ICD codes
- Missing documentation
- Failure to verify insurance eligibility
- Delayed claim submission
- Ignoring denied claims
Professional billing services for mental health clinics help identify and correct these issues before they impact revenue.
The Growing Demand for Mental Health Billing Services in USA
With increasing awareness around mental health, more providers are entering the field.
This growth has led to:
- Increased competition
- Higher administrative demands
- Greater need for compliance
As a result, mental health billing and credentialing services are becoming essential rather than optional.
Before You Decide: Build a Strong Financial Backbone
If you're running a mental health practice, your success depends not just on clinical expertise but also on financial stability.
Integrating professional medical billing and coding services along with reliable credentialing services can transform how your practice operates.
A Note on Trusted Support
Many providers today are exploring experienced partners like 247 medical billing services to streamline their operations. With expertise in medical billing services, medical coding services, and comprehensive revenue cycle management services, such providers help practices reduce administrative stress while maintaining compliance.
By combining advanced tools with industry knowledge, they also offer dependable credentialing services, ensuring providers stay connected with major insurance networks.
Conclusion
Mental healthcare is too important to be slowed down by administrative inefficiencies. Whether you're a solo therapist or managing a large clinic, investing in the right mental health billing services can unlock growth, improve cash flow, and enhance patient care.
From accurate coding to seamless credentialing, every step plays a role in your success. By embracing professional support and modern billing solutions, providers across the USA can focus on what truly matters—helping people lead healthier lives.
FAQs
1. What are mental health billing and credentialing services?
They include managing insurance claims, coding, payments, and enrolling providers with insurance companies to ensure smooth reimbursements.
2. Why should I outsource mental health billing?
Outsourcing reduces errors, improves revenue, saves time, and allows providers to focus on patient care instead of administrative tasks.
3. How does credentialing affect my practice?
Without proper credentialing, you cannot bill insurance companies, which directly impacts your revenue.
4. What is the difference between medical billing and coding?
Coding translates services into standardized codes, while billing uses those codes to create and submit claims for payment.
5. Are mental health billing services expensive?
Costs vary, but many providers find outsourcing more cost-effective than maintaining an in-house billing team.
6. Can billing services help reduce claim denials?
Yes, experienced billing professionals identify errors early and ensure accurate submissions, significantly reducing denial rates.