Mental health professionals across the USA are doing more critical work than ever before—but behind every therapy session lies a complex administrative process that can quietly drain time, revenue, and energy. Billing for mental health therapists is not just about submitting claims; it’s about navigating insurance rules, coding accurately, and ensuring consistent cash flow.
For many practices, especially solo therapists and small clinics, billing can become overwhelming. This is where structured systems and expert support—like mental health insurance billing services—can make a significant difference.
In this guide, we’ll break down how mental health billing works, the challenges therapists face, and how modern solutions can simplify the entire process.
Understanding Billing for Mental Health Therapists
Billing in mental health is uniquely complex compared to other medical fields. Therapists deal with varying session lengths, evolving treatment plans, and frequent insurance policy updates.
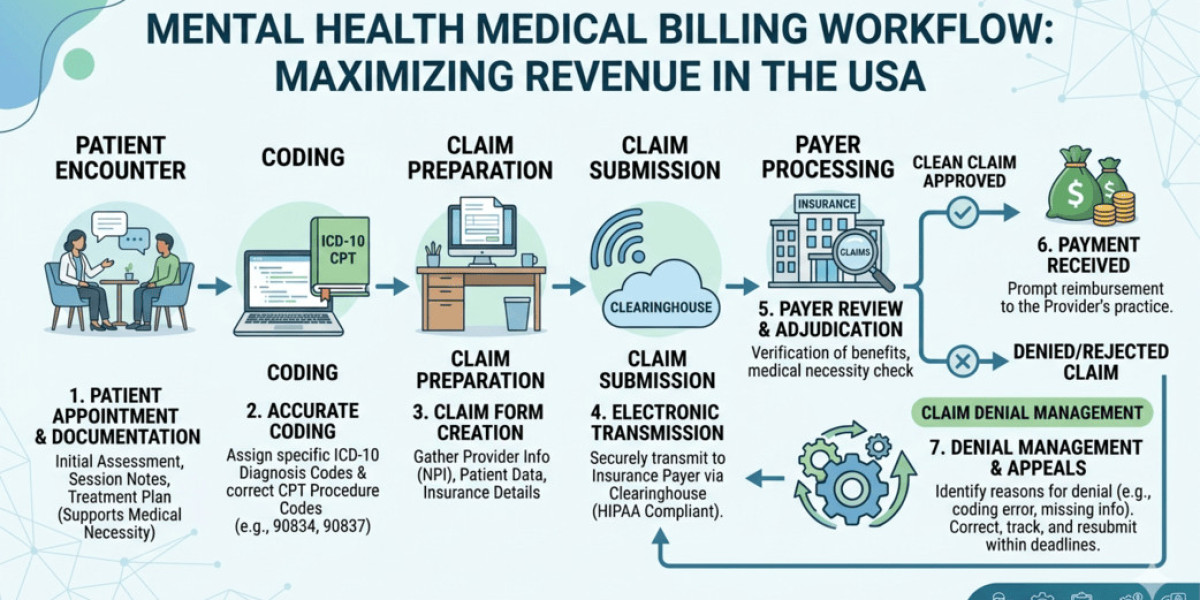
At its core, billing involves:
- Verifying patient insurance eligibility
- Assigning correct CPT and ICD-10 codes
- Submitting claims to insurance providers
- Handling claim rejections and denials
- Managing patient billing and collections
Even a small error in coding or documentation can lead to delays or revenue loss.
That’s why many providers turn to a mental health billing specialist who understands the nuances of therapy-based services.
Why Mental Health Billing Is More Challenging Than You Think
Unlike standard medical procedures, therapy sessions don’t always follow fixed patterns. This variability introduces complications in billing.
Key Challenges:
1. Frequent Coding Updates
Mental health billing relies heavily on precise coding. Incorrect use of CPT codes can result in denied claims.
2. Insurance Limitations
Many insurance plans impose session limits or require pre-authorizations, making billing more complex.
3. High Denial Rates
Errors in documentation or coding often lead to claim rejections.
4. Time-Consuming Follow-Ups
Tracking unpaid claims and resubmitting them takes valuable time away from patient care.
Because of these hurdles, therapists increasingly rely on mental health medical billing services to ensure accuracy and efficiency.
The Role of a Mental Health Billing Specialist
A mental health billing specialist acts as the backbone of your revenue process. They handle the administrative workload so therapists can focus on patient care.
What They Typically Do:
- Verify insurance benefits before sessions
- Assign accurate billing codes
- Submit claims electronically
- Monitor claim status and follow up
- Resolve denials and appeals
- Generate financial reports
Having a specialist ensures that billing is not just done—but done right.
Benefits of Outsourcing Mental Health Billing Services
Outsourcing has become a preferred solution for many practices looking to scale efficiently without increasing administrative burden.
Why Practices Choose to Outsource:
✔ Reduced Administrative Stress
Therapists can focus entirely on clinical work.
✔ Improved Revenue Cycle
Faster claim submissions and fewer errors lead to quicker payments.
✔ Cost Efficiency
Hiring an in-house team can be expensive. Outsourcing reduces overhead.
✔ Access to Expertise
A mental health billing and coding company brings industry-specific knowledge.
✔ Better Compliance
Staying compliant with HIPAA and insurance regulations becomes easier.
Outsourced mental health billing is especially beneficial for growing practices that want to maintain consistency without expanding internal teams.
Choosing the Best Mental Health Billing Agency
Not all billing partners are created equal. Selecting the right mental health billing agency can directly impact your financial performance.
What to Look For:
Experience in Mental Health
General billing agencies may not understand therapy-specific requirements.
Transparent Pricing
Avoid hidden fees or unclear billing structures.
Technology Integration
Ensure compatibility with your EHR system.
Strong Reporting System
Access to real-time analytics helps track performance.
Responsive Support Team
Quick issue resolution is critical for maintaining cash flow.
A top outsource mental health billing company will act as a partner—not just a service provider.
How Mental Health Medical Billing Services Improve Cash Flow
A well-managed billing system ensures that claims are processed quickly and correctly.
Key Improvements:
- Faster reimbursements
- Reduced claim denials
- Accurate coding practices
- Streamlined documentation
- Better patient billing transparency
By leveraging a mental health medical billing solution, practices can significantly increase their revenue without increasing workload.
Real-World Example: A Growing Therapy Practice
Consider a mid-sized therapy clinic in Texas that was struggling with delayed payments and frequent claim rejections.
After switching to outsourced mental health billing services:
- Claim approval rates increased by 30%
- Revenue cycle time reduced by 40%
- Administrative workload dropped significantly
The clinic was able to focus more on expanding services instead of chasing payments.
The Importance of Billing Services for Mental Health Providers
Reliable billing services for mental health providers ensure consistency and financial stability.
Core Functions Include:
- End-to-end claim management
- Denial tracking and resolution
- Insurance communication
- Patient invoicing
- Financial reporting
Without a structured system, even established practices can face revenue leakage.
Integrating Medical Billing and Coding Services into Mental Health Practices
While mental health billing is specialized, it still relies on broader systems like medical billing services and medical coding services.
Why Integration Matters:
- Ensures consistency across all healthcare services
- Improves coding accuracy
- Reduces compliance risks
- Enhances overall workflow efficiency
Medical billing and coding services form the foundation of an effective billing ecosystem, especially when combined with mental health-specific expertise.
The Role of Revenue Cycle Management Services
Revenue cycle management services go beyond billing—they oversee the entire financial journey of a patient.
This Includes:
- Patient registration
- Insurance verification
- Charge capture
- Claim submission
- Payment posting
- Denial management
For mental health practices, strong revenue cycle management ensures predictable income and long-term growth.
Why Credentialing Services Matter for Therapists
Before a therapist can bill insurance providers, they must be properly credentialed.
Credentialing services help with:
- Enrolling with insurance networks
- Maintaining compliance
- Updating provider information
- Avoiding billing delays
Without proper credentialing, even correctly submitted claims may be rejected.
The Future of Mental Health Billing in the USA
The mental health industry is rapidly evolving, and billing practices are changing alongside it.
Emerging Trends:
- Increased use of automation and AI tools
- Telehealth billing expansion
- Value-based care models
- Enhanced data analytics
Mental health billing companies are adapting to these changes by offering more advanced, tech-driven solutions.
Final Thoughts
Billing for mental health therapists in the USA is no longer just an administrative task—it’s a strategic component of practice growth. With increasing demand for therapy services, having an efficient billing system is essential.
Whether you choose in-house management or outsourced mental health billing, the goal remains the same: accuracy, efficiency, and consistent revenue.
Providers looking for reliable support often explore solutions offered by companies like 247 medical billing services, which combine expertise in medical billing services, medical coding services, medical billing and coding services, and revenue cycle management services. Along with credentialing services, such integrated support systems help mental health practices operate smoothly without compromising on care quality.
FAQs
1. What is billing for mental health therapists?
It refers to the process of submitting therapy session claims to insurance companies, including coding, documentation, and payment tracking.
2. Why should I outsource mental health billing services?
Outsourcing reduces administrative burden, improves claim accuracy, and ensures faster reimbursements.
3. How does a mental health billing specialist help?
They handle coding, claim submission, denial management, and ensure compliance with insurance guidelines.
4. What are the benefits of mental health medical billing services?
They improve cash flow, reduce errors, and streamline the entire billing process.
5. How do revenue cycle management services support therapists?
They manage the entire financial lifecycle—from patient registration to final payment—ensuring consistent revenue.
6. Do therapists need credentialing services?
Yes, credentialing is essential to get approved by insurance providers and receive reimbursements.